The Nipah virus is a zoonotic pathogen that has quietly circulated in fruit bat populations for decades, but when it spills over into humans, it can cause outbreaks with devastating consequences. With recent cases detected in Kerala, India triggering airport screenings across Asia, understanding how this virus works has become more crucial than ever. This deadly pathogen represents one of the most concerning emerging infectious diseases due to its high fatality rate, ability to spread between people, and the absence of specific treatments or vaccines.
How Nipah Virus Spreads from Animals to Humans
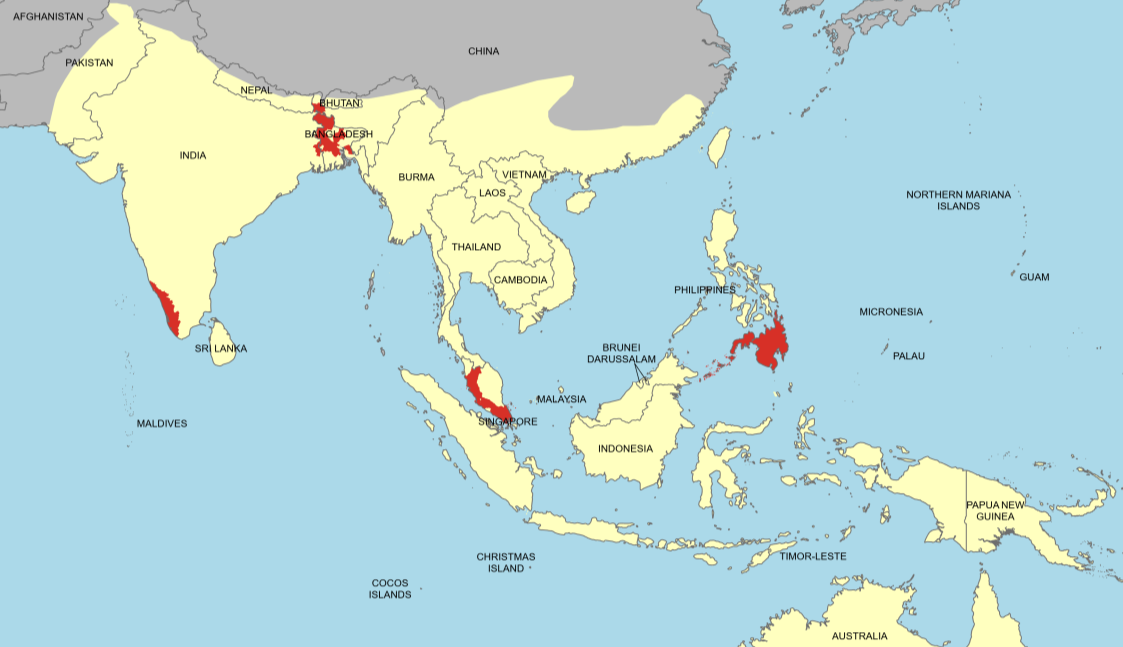
Nipah virus operates through a complex transmission chain that begins with fruit bats of the genus Pteropus, commonly known as flying foxes. According to the CDC, these bats serve as the natural reservoir hosts, carrying the virus without showing symptoms. The spillover to humans typically occurs through two primary routes: consumption of contaminated food or direct contact with infected animals.
"People can be infected with Nipah from direct contact with infected animals, like bats or pigs, or by consuming food or drinks, like fruit or raw date palm sap, that are soiled by infected animals," explains the CDC fact sheet. The virus can contaminate date palm sap when bats feed on the collection pots, creating a direct pathway to humans who consume the raw sap. Once the virus jumps to humans, it can then spread through close contact with body fluids of infected individuals, creating chains of human-to-human transmission that have fueled outbreaks in healthcare settings.
The Timeline of Nipah Infection: From Exposure to Severe Symptoms
Understanding the progression of Nipah virus infection requires looking at its incubation period and symptom development. The World Health Organization notes that the incubation period ranges from 4 to 14 days, though it can occasionally extend to 45 days. This extended window makes containment challenging, as exposed individuals might not show symptoms for weeks.
The initial phase typically presents with influenza-like symptoms including fever, headache, muscle pain, vomiting, and sore throat. "People with Nipah are typically sick for 3 to 14 days with fever, headache, cough, sore throat, and difficulty breathing," according to CDC guidance. What makes Nipah particularly dangerous is its potential progression to encephalitis - inflammation of the brain - which can develop rapidly. Patients may experience dizziness, drowsiness, altered consciousness, and seizures, potentially falling into a coma within 24-48 hours of neurological symptom onset.
Diagnosing and Treating Nipah Virus Infections
Diagnosing Nipah virus presents significant challenges, particularly in regions where healthcare resources are limited. The WHO explains that diagnosis typically involves laboratory testing of samples including throat swabs, cerebrospinal fluid, urine, and blood. Real-time polymerase chain reaction (RT-PCR) tests can detect viral RNA during the early stages of illness, while antibody detection methods become useful later in the course of infection or during recovery.
Perhaps the most sobering aspect of Nipah virus is the current state of treatment options. "Currently there are no licensed treatments for Nipah," states the CDC clearly. "Treatment is limited to supportive care, including rest, hydration, and treatment of other symptoms." This supportive care focuses on managing fever, maintaining hydration, addressing respiratory distress, and controlling neurological symptoms. The absence of specific antiviral therapies underscores why prevention and early detection remain the most effective strategies against this pathogen.
Prevention Strategies: Breaking the Transmission Chain
Preventing Nipah virus transmission requires a multi-layered approach targeting each point in the transmission cycle. The WHO emphasizes several key strategies for reducing infection risk:
- Reducing bat-to-human transmission: Using protective coverings on date palm sap collection sites, boiling freshly collected sap, and thoroughly washing and peeling fruits before consumption
- Reducing animal-to-human transmission: Wearing protective equipment when handling sick animals and implementing biosecurity measures on farms
- Reducing human-to-human transmission: Practicing regular hand hygiene, using personal protective equipment when caring for patients, and implementing isolation protocols
For healthcare workers, the WHO recommends contact and droplet precautions including medical masks, eye protection, fluid-resistant gowns, and gloves. During aerosol-generating procedures, airborne precautions with fit-tested respirators become essential. These measures proved critical during the 2018 Kerala outbreak, where healthcare worker infections highlighted the virus's capacity for nosocomial spread.
Recent Outbreaks and Global Health Response
The pattern of Nipah outbreaks has evolved since the virus was first identified in 1999 during an outbreak in Malaysia and Singapore that affected pigs and pig farmers. Today, Bangladesh and India experience near-annual outbreaks, with Kerala reporting its fifth outbreak in six years in July 2024. The recent detection of cases among healthcare workers in West Bengal has triggered airport screenings across Asia, reflecting the global concern about this pathogen's spread.
"WHO has identified Nipah virus infection as a priority disease for the WHO Research and Development Blueprint," indicating its status as a pathogen with epidemic potential. This designation has accelerated research into diagnostics, therapeutics, and vaccines, with several candidate products now in various stages of development. The international health organization works closely with at-risk countries to strengthen surveillance, clinical management, laboratory capacity, and community engagement.
The Future of Nipah Virus Control and Research
Looking forward, the battle against Nipah virus focuses on several key fronts. Vaccine development represents the most promising long-term solution, with several candidates showing progress in clinical trials. The University of Oxford launched the world's first Phase II clinical trial of a Nipah virus vaccine candidate in December 2025, marking a significant milestone. Meanwhile, research continues into antiviral therapies that could improve outcomes for infected individuals.
Surveillance and early detection systems are being strengthened in endemic regions, with improved laboratory capacity and faster diagnostic tools. Community education programs emphasize the risks of consuming raw date palm sap and the importance of avoiding contact with sick animals. As climate change and habitat encroachment potentially alter bat migration patterns and human-bat interactions, these prevention strategies will become increasingly vital.
Key Takeaways for Understanding Nipah Virus
The Nipah virus represents a perfect storm of concerning characteristics: high fatality rates, multiple transmission routes, and limited treatment options. Yet understanding its mechanics provides a roadmap for prevention. The virus's dependence on specific ecological conditions - particularly its reservoir in fruit bats and transmission through date palm sap - creates targeted opportunities for intervention. While the recent outbreaks have rightly raised concerns, they have also spurred unprecedented international collaboration and research investment.
For now, awareness remains our most powerful tool. Recognizing the symptoms, understanding the transmission routes, and implementing basic prevention measures can significantly reduce infection risks. As research advances toward vaccines and treatments, the global health community continues to monitor this pathogen closely, applying lessons learned from each outbreak to strengthen our collective defense against this deadly virus.


